THE CRUELEST
EQUATION
Do nothing and this rarest
of diseases would kill her boys.
But the cure can kill too, already had. Could she risk a second son?
BY KATE HARRISON BELZ
PHOTOGRAPHY BY DOUG STRICKLAND
After the funeral, she stopped speaking to doctors.
She let calls from the pediatrician go to voicemail.
She stayed home during the checkups and the hospital visits.
The doctors kept telling Jasmine Latham that her 2-year-old would fare better than his brother, that the odds would be better the second time around.
But odds stopped meaning anything to Jasmine a long time ago.
ABOVE
Bryson Johnson wears a surgical mask to prevent infection as he sits with his mother, Jasmine Latham, on a hospital bed at Erlanger Hospital waiting to undergo an infusion of intravenous immunoglobulin in June of 2014.
“One in a million” was how doctors described the genetic disease called IPEX. Still, it found its way into two of her three sons.
“Normal,” the boys’ newborn screening tests had said. Yet one hidden, molecular glitch had triggered their bodies to self-destruct.
“Seventy five to 80 percent” were the chances the doctors gave her middle son of being healed by a bone marrow transplant. But he was gone.
And there was the cruelest equation: The same thing that might save her youngest son could kill him.
Science and medicine offered Jasmine no comfort. So she tuned them out. She made dinner for the boys and turned on cartoons. She drew hot baths, wanting to be cradled by warmth. She moved with dreamlike slowness through snow days and Easter egg hunts, pretending the sickness wasn’t always lurking in the background.
Psychologists call it denial, the refusal to accept harrowing truth.
But for Jasmine, denial was the only way to survive. The only way to bear the flashbacks of the tiny toddler in the hospital bed, swaddled in wires and tubes. The only way to find relief on the sleepless nights, when she ached for the little boy who used to crawl in under her sheets.
Denial was the only way to keep some sense of order in a world that had none, in a bizarre reality where math did not compute.
She was supposed to have three boys. Kaivon, Tré and Bryson.
Three boys: “My sun, my moon, and all my stars,” she always told them.
The lights of her life.
And now, inexplicably, there was darkness.
Bryson sits alone on a hospital bed playing video games on a tablet to keep him occupied as nurses prepare his injection of IVIG. While the treatment helps to keep Bryson healthy, the only known cure for IPEX is a bone marrow transplant, which has a 70-80% success rate.
ABOVE
THE
TIME
BOMB
ABOVE
Bryson's grandmother Melissa carries him from appointment to appointment during a regular visit to Erlanger, where he receives scheduled check-ups and injections to monitor and maintain his health. The family makes monthly visits for appointments to Chattanooga, where the hospital is located, from Sweetwater, which is about an hour away.
Families facing rare genetic disease live on a lonely and desperate frontier.
Twenty years ago, mothers like Jasmine had no idea why their seemingly perfect babies kept getting sick. Infections would attack suddenly, and kill without explanation.
Only now are some of the answers beginning to surface. Exploration of the human genome has unlocked long-hidden mysteries of hereditary illness. New genetic mutations — and the illnesses they unleash — are found every year. IPEX syndrome, the deadly autoimmune disease that two of Jasmine’s boys were born with, was identified only a dozen years ago. Even the boys’ pediatricians had never heard of IPEX before their diagnosis.
Yet while new discoveries bring hope, they also create impossible dilemmas. Scientists may be able to pinpoint a genetic malady in a child. But that doesn’t always mean they know how to heal it. Most genetic disorders have no cure. How should parents proceed?
There is no map, no well-beaten path to show the next step. Do you try new or experimental treatments, knowing full well the risks they may carry? Or do you wait — for new science, for a new experimental drug, or a miracle?
Treatments, if they exist, are exorbitantly expensive, and often require crisscrossing the country or the globe. Children may be treated by scores of doctors in a given year. Normal life becomes a vague memory. Parents quit jobs. They disappear from friends and family, consumed by a constant barrage of medical demands. Crisis becomes customary.
For the rarest of disorders, there are no support groups. There are no foundations or walkathons. There is no pressure on drug companies to find a cure.
So mothers like Jasmine are left to cope alone, forced to make choices that have no precedent.
At times she can tell herself nothing is wrong. Her boys squabble and squeal and careen down the sidewalk on tricycles, like little boys should.
But the truth is always there, no matter how far she shoves it to the back of her mind.
Her baby is a ticking time bomb.
THREE BOYS,
ONE MYSTERY
ABOVE
Jasmine watches Bryson as he climbs around the living room while watching television at their home in Sweetwater, Tenn., in October of 2014. Bryson's health is always in question, and could deteriorate rapidly even with treatment.
Sweetwater, Tenn., is a town situated in the foothills of the Great Smoky Mountains and surrounded by farmland. It’s a town where everyone knows everyone.
Melissa Latham grew up there, and decided to stay to raise her two daughters there, too. She brought them up on her own after she and their father divorced, working as a nurse to support the family.
Jasmine was the youngest, freckled and curly-haired. She was a cheerleader at Sweetwater High, and worked at Burger King after school. When she was 16, she started dating a boy she had gone to school with since fifth grade, one of her best friends. She was in love, but she had plans to go to college to study criminal justice.
Then, her senior year, she found out she was pregnant.
She told her mother she was scared. At 17, she was too young to care for a child. Too selfish. She liked staying out with her friends. She liked her cheerleader body. She liked her sleep.
You’ll learn, said her mother, always matter-of-fact.
And in November 2009, when Jasmine finally held her tiny blanketed bundle, Kaivon Jarrell, she began to understand.
Months later she was pregnant again, with another boy she would call Tré Alexander. And when she was 20, she found out she was going to have a third son.
Some people told her to get an abortion, or put the third baby up for adoption.
You know you’re going to be raising them alone, they said.
Though the boys had the same father, Jasmine was raising them on her own. She had stayed with him for a long time — thinking in the back of her mind that they might get married one day. But he wouldn’t stick around.
Still, Jasmine could not fathom giving up this third child. Bryson Tyrese arrived in September 2011.
Jasmine was just learning to maneuver school, work and motherhood when two of her boys began showing strange signs.
Tré, the middle son, wasn’t growing right— at least not like Kaivon had. At 7 months, Tré wasn’t putting on weight. He had chronic, watery diarrhea. He slept all day. And when he was 8 months old, he quit breathing.
His face turned blue, and Melissa, who was watching him, found nothing blocking his airways. She started rescue breathing, her mouth to his. It took 45 minutes for doctors at the Sweetwater hospital to stabilize him. Afterward, they couldn’t say for sure what happened. It seemed like a physiological fluke. A one-time thing.
But it happened again, and again, more rattling each time. Doctors kept saving him, but they couldn’t figure out what was wrong.
The youngest son’s poor health was just as puzzling. Bryson came down with double pneumonia, then a kidney infection. As he grew, the list of his allergies grew, too: Milk. Wheat. Soy. Eggs. Peanuts. Pineapple.
When the boys tried day care, their illnesses only multiplied. A simple virus sent their bodies into a tailspin. Ear infections, respiratory infections. Back to the hospital they would go. The oldest son, Kaivon — who remained as healthy and rambunctious as ever — would tag along, tearing through the hospital as if he owned the place.
Every new month brought a new antibiotic. Someone anonymously reported the family to the Department of Children’s Services for how often the boys were getting sick. Melissa was furious.
The grandmother, with her nurse’s instincts, was sure there was something deeper going on with her boys, and she kept telling the doctors so. In the summer of 2012 she and Jasmine began driving an hour south to T.C. Thompson Children’s Hospital at Erlanger in search of answers.
ABOVE
Jasmine comforts her healthy son, Kaivon, Bryson's older brother, as he throws a tantrum in a waiting room during one of their visits to Erlanger Hospital while her mother Melissa holds Bryson in July of 2013. The constant attention paid to his sick siblings sometimes causes Kaivon to act out for attention of his own.
It was there the Lathams first met Dr. Kourtney Santucci, a pediatrician who specialized in rare disorders, and who had always been drawn to the toughest cases. Santucci sensed the brothers were not just sickly. Too many different body systems had been assaulted. She suspected some kind of orchestration behind it all, as if the boys’ bodies were obeying some perverse order to self-destruct.
But tests revealed nothing. They were negative for HIV. Negative for cystic fibrosis, negative for lupus. Negative for a dozen other diseases.
The boys needed to be looked at by higher-level experts, Santucci decided. So she pushed for them to travel to the Cincinnati Children’s Hospital, a national leader in diagnosing genetic maladies.
The problem was how to pay for it. The tests alone would be thousands of dollars, plus travel. Jasmine had quit both school and work to care for the boys full time. The kids were insured through Tennessee’s Medicaid program, TennCare, but the agency traditionally did not allow for treatment out of state.
But when Santucci wrote the agency, telling representatives it was life or death, they agreed to the tests. The family drove to Ohio in January 2013, and braved a gauntlet of pricks, scrapes and extractions to produce enough fluids and tissues for the tests.
Five months passed before a doctor from Cincinnati called, saying they found something in Tré’s and Bryson’s tests: A very peculiar mutation on a very particular gene. It was a disease called IPEX syndrome, the doctor on the phone explained. The strange name was more comprehensible than the things he said next:
It is a genetic disease.
It affects only boys.
It is extremely rare.
Only 150 to 200 people in the entire world have been diagnosed with it.
And most boys with IPEX don’t live past their third birthdays.
THE
FAMILY
CURSE
ABOVE
Jasmine holds down Bryson and tries to comfort him as a nurse draws blood during a July 2013 visit to Erlanger. Jasmine said that at first it was very difficult for her to watch procedures performed on her children or stay with them in the hospital, but over time it has become easier.
Googling IPEX was pointless.
Searches turned up a plastics manufacturer, a global printing company, the European Union’s interparliamentary exchange. The few research articles on the disease were mind-numbing.
The Lathams had crossed into medical borderlands, into territory few researchers had explored.
The quest to understand IPEX began about 30 years before the boys were born, with an Oregon pediatrician named Dr. Berkely R. Powell, who with a team of researchers was trying to solve a family curse.
In 1975, Powell cared for a baby boy with severe diarrhea, who died at just 7 months old. Talking with the boy’s mother, he learned that many other boys in the family — at least 17, he later found — had died in early childhood, plagued by problems like diabetes, anemia or chronic diarrhea.
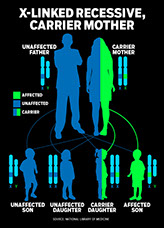
Drawing out the family tree, Powell found that the sick boys were all linked by blood through women in the family — proof that the deadly inheritance, whatever it was, passed from the mothers’ X-chromosomes to their sons.
Powell’s team was able to show that the disorder was genetic, and that it involved the immune system’s cells. But the root cause was still unclear.
Hopefully by the time your daughter is grown up and ready to have children, Powell told the first patient’s mother, scientists should know the cause for this.
Two more decades would pass before researchers actually nailed the culprit: A single, mutated gene called Forkhead Box P3. The FOXP3 gene — as it was nicknamed — pumps out the code needed to build a key protein found in the thymus gland. There, behind the lungs, that protein helps to manufacture immune system cells called regulatory T cells.
If the immune system is a squad of battle-hungry assassins, programmed to hunt down and kill any threats, then regulatory T cells are the commanders, telling them to put the gun down once the mission is accomplished.
But a mutation of FOXP3 triggers a chain reaction that leaves boys like Tré and Bryson short on regulatory T cells. Unchecked, the immune system not only fails to protect the body from infection — it turns trigger-happy and treasonous, attacking the body’s own tissues and organs in all-out mutiny.
Boys with IPEX often appear normal and healthy. It’s both a blessing and a curse, parents say. They have a hard time convincing friends, even new doctors, that something is wrong.
But the illness breaks the boys’ bodies down as they get older. The children who die of IPEX often die of “overwhelming autoimmunity” — meaning the body destroys itself. It could look like kidney failure, or the inability to retain nutrients, or a sudden infection.
Scientists decided to name the syndrome after its telltale symptoms: Immune dysregulation, polyendocrinopathy, enteropathy, X-linked. Shortened, it sounded more like a villain from a science fiction movie: IPEX. Against such a villain, little boys stood little chance.
Jasmine often envied the ignorance of the parents who had never known what took their children. The mystery was terrifying. But it seemed more unbearable to know her boys had been marked, that a tiny misprint in a tiny script of genetic code had doomed them before they were even born.
SEE HOW IPEX
IS PASSED FROM
GENERATION
TO GENERATION
A CURE AND
A RISK
ABOVE
Bryson, right, plays with his older brother Tré in a playground courtyard during a visit to Erlanger about 8 months before Tré died after complications from a bone marrow transplant in Cincinnati to treat his IPEX. Jasmine is now faced with the decision of whether or not to put Bryson through the same procedure that took his brother's life.
There was one way to save the boys, doctors told Jasmine: A bone marrow transplant.
They could fight the disease with pills and monthly infusions of pooled antibodies pumped into the squirming boys’ veins. But a transplant was the only thing that could swap out the treasonous immune system with one that worked.
The doctors all agreed Tré needed the transplant as soon as possible. He could test positive for diabetes or a kidney disorder any day. Flu season could be lethal.
But the transplant was also a gamble, with a 70 to 80 percent success rate for IPEX kids. Of 20 known IPEX patients transplanted in the United States, six died during the process.
Any number of things could go wrong during the transplant: His kidneys could shut down. The new cells could turn on him in what’s known as graph-versus-host.
Jasmine wrestled with doubts. In the summer of 2013, Tré looked the healthiest he had ever been. But her fears were always overruled by the inevitable verdict: If Tré or Bryson had any hope of surviving childhood, it would be through transplant. There was no choice.
Tré would go first, then Bryson, they decided. The transplants for both boys had to be done in Cincinnati. No Tennessee hospitals were equipped to transplant a kid with IPEX. And that meant the Lathams would have to leave Sweetwater for at least a year. The full process of each transplant would take six months or longer. After some back and forth, TennCare agreed to pay for the treatment and for a Best Western hotel room for the family to live in during the treatment. Melissa had to quit her job and Jasmine gave up her apartment. Some friends organized fundraisers, but the family had little to live on.
The mother-daughter duo decided that Melissa, with all of her nurse experience, would stay with Tré in the hospital. They would be totally isolated. Tré’s immune system would be too vulnerable for him to leave his room. Jasmine, meanwhile, would set up a makeshift home in the Best Western with the other boys. Kaivon was almost 4 years old, and bursting with energy. Bryson was just learning to talk. The family stuffed the car with clothes and toys and movies — enough, they hoped, to get them through the long year.
Doctors call the day a patient gets a bone marrow transplant Day Zero — a new birthday of sorts, with brand-new cells. For Tré, Day Zero was Sept. 13, 2013 — a month before he turned 3.
Jasmine cried the whole morning, while nurses hung a banner in Tré’s room. It bore the words “Happy Cell Day Tre!” flanked by images of Woody and Buzz Lightyear from “Toy Story.”
Tré was running back and forth on the hospital bed, tapping the machinery, asking, “What’s dis? What’s dis?” He erupted in a high-pitched giggle, hands to his mouth.
As the toddler was hooked up to a series of tubes, the hospital chaplain prayed a blessing over the bag of new blood cells that would be siphoned into his body. Jasmine stood beside Tré for the next two hours as the blood drained from the bag. I love you, she said through tears, over and over. I love you. I love you. I love you.
HOW A BONE MARROW TRANSPLANT WORKS
ABOVE
Jasmine stands by Tré as his bone marrow transplant is administered through an infusion at Cincinnati Children's Hospital in September, 2013.
Weeks passed, and Tré’s dark curls began to fall out in patches. His face and belly ballooned from the steroids ingested to help his body adjust to the new cells. But Tré’s outlook appeared promising. On Oct. 5, he was 100 percent engrafted — meaning the transplanted stem cells had found their way to the marrow within his bones, where they could begin making new blood cells.
“Tré will get through this just fine,” Melissa wrote on the boys’ Facebook page. “He still is our little fighter.” She posted a photo of him in a shirt with superheroes on it.
The days were long and lonely. Jasmine was cooped up in the hotel with the other boys, and saw Tré only an hour or two a day. In the hospital, Melissa had no room to herself. She showered in a public hospital stall and ate at cafeteria tables she had to wipe down before and after eating. The fear of germs ruled life in the transplant unit. Isolated as they were, families in the unit seemed to avoid contact with each other. Melissa saw the faces of parents grow haggard and haunted over the long weeks. They reflected her own.
One day Melissa saw Tré staring through the window of his room. Another little boy stood across the hallway. A nurse came and scooped the other boy up, and held him to the window. Tré pressed his palms against the glass. The boy on the other side did the same. Melissa fought back tears.
Mother and grandmother celebrated every small victory. There was the day Tré got to eat roast beef. Days he got to leave his room. When he turned 3 on Oct. 20, he unwrapped a set of new toy airplanes.
But there were bad days, too. Days when Tré’s cell counts were off, or days when searing pain had to be dulled with morphine. Days his nose bled all day.
ABOVE
Hospital staff created a banner to celebrate Tré's new "cell day," or "Day Zero" — the day he will be given a donor's bone marrow to help his body create new, healthy immune system cells.
ABOVE
Jasmine and Melissa stand with Tré in the ICU after he was baptized in December 2013. At this point he had been put on a ventilator as his condition continued to go downhill.
And, over the weeks, the bad days multiplied. Around the end of November Tré’s kidneys began to fail and he was put on dialysis. Viruses swept into his body; he ran a high fever. His lung collapsed when doctors tried to replace a breathing tube. High levels of carbon monoxide were found in his blood. Melissa grew more and more frustrated with the doctors, afraid they did not truly understand IPEX.
In December, doctors put Tré on a ventilator. Tubes webbed his round belly and his swollen baby cheeks, into his mouth and his nostrils. The steady whoosh of the breathing machine kept pace with the plea throbbing through mother and grandmother: Live, live, live. Please live.
Jasmine decided to have Tré baptized. The chaplain dipped a seashell into water and sprinkled it over the unconscious toddler. The family prayed for a miracle. Maybe impossible odds would be in Tré’s favor this time.
Jasmine stopped eating. Later that month, Melissa sent her daughter back to Sweetwater, where she was hospitalized. The doctors there told Jasmine her lab work looked like that of someone who was starving to death. She was showing symptoms of post-traumatic stress disorder. The doctor prescribed her a diet regimen and anxiety medicine before she headed back up to Ohio.
Melissa’s Facebook posts became more heavy-hearted.
“Tré is in very critical situation. … We love Tré with everything we have. … We appreciate all the prayers! God knows our desires; His will be done. Drs may make mistakes but God does not.”
One afternoon a social worker brought a bowl of plaster into the room. Jasmine clasped Tré’s hand while the social worker coated their fingers with the doughlike goo. The plaster mold would be turned into a small sculpture of this moment: Mother and son, holding fast. Not ready to let go.
As the weeks went by, as Christmas and New Year’s came and went, Tré began to slip away.
On Jan. 18, 2014, he let go.
ABOVE
A casting of Jasmine's hand holding Tré's, and another of Tré's fist. Hospital workers helped Jasmine make the castings as Tré's outlook worsened towards the end of 2013.
THE
QUESTION
OF WHY
ABOVE
A pinwheel that has been placed on Tré's grave spins next to his headstone, where other mementos have been left by his family.
When she got home to Sweetwater, Jasmine did not want to see anyone. She knew what they would all say: “I’m so sorry.” “It’s going to be OK.” “I’m here for you.” “You’re so strong.”
None of that is true, she thought.
The people of Sweetwater had long prayed that the Lathams would return from Cincinnati toting a healthy boy. When they came home with a small white casket, the town grasped for ways to rally around them.
Jasmine’s best friend organized a candlelight vigil. A tire store gave money to buy candles. Sweetwater High School loaned projectors and speakers. A local print shop donated 500 programs. A stylist in Sweetwater did Jasmine’s hair for free, and she got a manicure: Red polish with the black letters “T-R-E” painted across her thumb.
As much as the outpouring moved her, Jasmine spent that Wednesday dreading the service. She arrived at the park with Melissa and the boys as darkness fell. The cold had set in.
DEALING WITH LOSS
Jasmine talks about the challenges she faced in the months following Tré's death, and how she struggled to cope with the loss of her son.
ABOVE
A friend hugs Jasmine at the close of a candlelight memorial service which was held for Tré at Engleman Park in Sweetwater on January 22, 2014. Jasmine later remarked that she could barely remember the experience, or the friends who came to comfort her, because she was so numb.
A slideshow began and Tré’s face beamed onto the screen: Baby Tré with a pacifier. Tré dressed up like a dinosaur. Tré playing in the pool. Tré holding his mother’s hand in the Cincinnati hospital.
The preacher got up to speak. In times such as these, he said, there are always questions. The biggest one is why. Why an innocent little boy? “This world is a sin-cursed world,” he said. “We don’t have the answers now.” But Tré was in heaven with God now, he said, free of IPEX.
It was hard for Jasmine to think about God. Why would he put her through this? Why would he take her baby?
And yet she found comfort thinking of Tré in heaven. He could run through gardens and play with angels, until they could meet again.
And I will hold him just like I did the day he left me, she thought. The only difference will be I won’t have to let go.
Jasmine’s uncle got up to speak. “Tré knew he was loved,” he said. “That love was handed down from his mother. And she got it from her mother.”
Passed down like a genetic imprint.
The crowd in the pavilion clutched their candles as wind swept through the park, lights flickering against an endless dark.
NOT
AGAIN
ABOVE
Jasmine, Bryson, Jasmine's sister Candice, their mother Melissa, and Kaivon, from left, light candles in memory of Tré as a slideshow plays on a projector during the memorial service.
Little came into focus for Jasmine after Tré’s death except one thing: She would not transplant her other sick boy.
It was for Bryson’s best, she reasoned. No matter how many days the 2-year-old had left, she wanted them to be free and happy. She wanted him to have swing sets and balloons and chicken nuggets. But she knew the decision was for her own sake, too. She could not face that hell again. She did not have the fight in her.
Jasmine moved out of Sweetwater, away from her friends and family, to an apartment in Athens, Tenn. She didn’t answer the phone when her mother called. She left her hair in a mess and went to the store in sweatpants. When they went out, Kaivon would tell strangers that his brother was in heaven. Jasmine never knew what to say.
The first day Jasmine and Melissa went to meet Bryson’s new pediatricians at Erlanger, Dr. Karla Garcia and Dr. Julia Katsuura, Jasmine sat in the room silently, not making eye contact with either doctor. As she went mute about Bryson’s illness, Melissa took charge of his medical care, driving him to Chattanooga a few times every month for checkups and four-hour infusions at Erlanger.
Bryson was used to hospitals by now. At the visits, nurses attached wires to his belly. “You’re a robot!” they told him. They scanned his heart, listening to the rhythms. “Is that a frog in your belly?” they asked. They turned on “Barney and Friends” while hooking up his IV.
They asked about Jasmine.
“Mom didn’t come today?” a nurse asked Melissa during one visit.
“Not today,” Melissa said.
“Is she doing OK?”
“I don’t know,” Melissa said, eyes focused on Bryson. “She never mentions his illness, never mentions his medicine. It’s like if she doesn’t say something, then it isn’t there.”
ABOVE
Cardiologist Dr. Gerald Johnson listens to Bryson's heart and lungs during a regular visit in June of 2014 as Bryson plays with a disposable ear specula.
In February, just a month after Tré’s funeral, a nasty virus sent Bryson back to the hospital. Jasmine was inconsolable.
What am I going to do if I lose two kids? she asked her mother.
For months, Melissa had tried to shield her daughter from such thoughts. But not this time.
You are going to lose two kids, Melissa said, meeting her daughter’s eyes. If he doesn’t have a transplant, that’s a definite.
But Melissa still had a stubborn hope. Like Jasmine, she was shaken by the idea of a transplant, but she wouldn’t rule it out. Doctors had caught IPEX much earlier in Bryson than they had in Tré, and the treatments were keeping him stable. He giggled, cried and roughhoused with his big brother. He was silly and flirtatious. He did headstands. He seemed unaware he was sick.
And there was someone Melissa still wanted to call about IPEX, a name that had come up again and again in her Google searches and Facebook chats with other IPEX families: Dr. Troy Torgerson.
Torgerson, a pediatrician at Seattle Children’s Hospital, had a reputation as one of the nation’s leading experts on IPEX. He had overseen 12 successful transplants for IPEX boys at Seattle Children’s, and was coordinating care for dozens of others across the country.
Melissa left a message with someone at the hospital, and was star-struck when Torgerson called her back. The doctor seemed warm and approachable and listened closely as she unloaded the last two years. He invited the family to come out to Seattle for a consultation.
It is still early for Bryson, he told Melissa. Lets see what we can do.
TennCare approved the Seattle trip for Bryson in May 2014. The family held a garage sale to help pay for plane tickets. The trip would be exploratory, they told friends and family. But Jasmine and Melissa both knew this was their one chance.
“Laying here in bed holding Bryson while he plays with The Wheels on the Bus app,” Jasmine posted to the boys’ Facebook page a few nights before the trip. “And I suddenly get teary eyed as I think … oh how I wish this Dr in Seattle could hug me and tell me it is ok that he can make Bryson all better and can promise he won’t die.”
ABOVE
Bryson climbs onto a chair as Dr. Johnson discusses his condition with his grandmother Melissa during their visit.
A SECOND
CHANCE
ABOVE
Bryson blows on a whistle necklace which Jasmine wears around her neck as she carries him back inside after playing outside at their home in Sweetwater.
Dr. Torgerson was well-acquainted with the agonies of IPEX.
He had arrived at Seattle Children’s Hospital as a young resident, right after the link between the FOXP3 mutation and IPEX was made. The disease had become his passion.
He forged close bonds with his patients. “My kids,” he called them. He had treated multiple children from the same families, some that spanned generations.
Sometimes he could intervene early. Babies whose siblings already had IPEX could be tested in the womb and given transplants after birth, before a single symptom showed up. On the other end of the spectrum, there were a handful of rare cases where young men had survived into their 20s before they were diagnosed and learned that transplant was an option.
In either case, the question of transplant came with its own anguish. But Jasmine’s dilemma was one of the most disturbing Torgerson had encountered. He spoke with the boys’ pediatrician by phone before the Lathams traveled west.
Jasmine is struggling, she told him. She might not talk to you.
The day Torgerson shook their hands in the Seattle hospital, Jasmine and Melissa immediately liked him. He wore a bowtie, and treated Kaivon and Bryson like little boys — “not like specimens,” Melissa thought. He seemed kind and yet blunt.
TWO LITTLE BOYS, MANY DOCTORS
See the network of specialists it takes to care for boys with IPEX.
ABOVE
Jasmine sits with Bryson on a hospital bed in Erlanger, arriving and taking over staying with him during his IVIG injection for her mother Melissa.
Torgerson sat down with the family and went over Bryson’s file. The boy was doing well. It was likely that his maintenance treatments could keep him relatively healthy for several years. But, he added, the longer they waited, the more the disease would progress.
Melissa asked him about gene therapy, the practice of re-engineering genes to cure disease. Torgerson told her such a cure could be anywhere from five to 15 years away, or longer. The best hope now — still —was bone marrow transplant.
Bryson has an excellent chance at survival, Torgerson explained to the mother and daughter.
But it was not 100 percent, he added. He could make no guarantees.
The doctor knew that a parent’s ability to endure transplant was just as crucial as the child’s. The process could cure a child, but destroy a family. The isolation, the turbulent weeks, the constant question of survival set parents up for nervous breakdowns. In a few extreme cases, he had seen mothers and fathers pack up and leave, abandoning their children to state custody.
When the doctor studied Melissa and Jasmine, he saw two mama bears. Jasmine, protective of her boys. Melissa, protective of her daughter. He saw the women were tough, but that their wounds were deep.
Let’s give it time, the doctor told them. You’re still in the grieving process. Bryson is managing OK, and we don’t have to rush.
Time. It was a new concept. And it could give them something they had lost since the IPEX first revealed itself: A moment to breathe.
ANOTHER DECISION LOOMS
Jasmine talks about continuing to raise Bryson, his uncertain future, and whether she will decide to go through with a bone marrow transplant.
GROWING UP
ABOVE
Jasmine and Bryson watch as a balloon he released floats away into the air in front of their home as Kaivon gets ready to let go of another.
It can be hard to notice healing. Time makes no sense in grief. Some days stretch out into long, aching blanks, while weeks can blend together in a haze. But in between them, Jasmine began finding moments of traction, steppingstones that proved her feet were still moving.
There was the family trip to Destin, Fla., where Kaivon and Bryson played on the beach and the family lit floating lanterns to send up to Tré. There was the day she moved back to Sweetwater, into her grandmother’s old clapboard house near the train tracks. She filled the walls with pictures of her three boys and with framed prints of her promise to them: “You are my sun, my moon, and all my stars.”
There was the day she went to Bryson’s doctor’s appointment, and one of the nurses cheered.
“You’re smiling!” she exclaimed to Jasmine. “Last time you were here you did not want to talk to me!”
ABOVE
Jasmine holds Bryson still as a nurse distracts him from an injection being inserted into his port by showing him how to blow bubbles.
After the visit with Torgerson, Jasmine began to accept the idea of Bryson having the transplant. She wanted to give him that chance. But every day she felt something different.
She and Melissa had become friends with other IPEX families on Facebook, a makeshift support group. Sometimes Jasmine sees the posts from parents slogging through the transplant journey — a child in the ICU, another child having trouble breathing — and she cannot sleep at night.
But then she sees other pictures of IPEX kids post-transplant. They look happy. They’re growing.
“Maybe that’s how it will go with Bryson,” Jasmine wrote on Facebook in November. “Then the memories and flashbacks of our experience with Tré come back and I get anxious all over … and I think, ‘that was my baby, he’s gone! I can’t do it again.’ … I don’t have to make a decision today, but when that time comes I know I won’t be ready for it.”
Another mother of an IPEX child wrote back. “Unfortunately no one can tell you what to do for Bryson,” she wrote. “But, you have faith, you have support, you have love, you have courage.”
In the time of uncertainty, Jasmine savors the mundane decisions — the normal dilemmas of childhood. Like what the boys would be for Halloween (a pirate and a Teenage Mutant Ninja Turtle). Or where to have birthday parties when Bryson blew out three candles and Kaivon blew out five (Chuck E. Cheese and the Tennessee Aquarium). There have been Christmas presents to pick out and arrange carefully under the tree.
There was the quiet night at home when Bryson could not decide whether he wanted to watch “Wreck It Ralph” or “Cars 2,” so Jasmine let him watch both. But the TVs were soon abandoned as the boys piled up the couch cushions to wrestle. They hollered and raced across the room while Jasmine watched from the doorway.
These are the moments when she just shakes her head and laughs.
The kind of moments in which, without thinking twice, she can imagine them as teenagers one day.
HELP BRYSON
BY DONATING
THROUGH
GOFUNDME
ABOUT THIS STORY
This story was reported and written over a period of 12 months. The narrative is based on extensive interviews with Jasmine and Melissa Latham and their sons’ physicians; hours spent with the family at doctors’ appointments and at their home; medical records and social media posts. Interviews with specialists and researchers across the country informed the reporting, as did medical research papers on IPEX and autoimmune disorders. Quotes italicized in the story were recounted to the reporter from a source who was present. Quotes in quotation marks were words heard by a reporter or taken from social media posts.
PHOTOGRAPHY BY
DOUG STRICKLAND
STAFF PHOTOGRAPHER
DESIGN BY
MATT MCCLANE
PRESENTATION EDITOR
STORY BY
KATE HARRISON BELZ
STAFF WRITER
PRODUCTION BY
MAURA FRIEDMAN | MARY HELEN MILLER | KEN BARRETT
GRAPHICS BY
LAURA W. MCNUTT
GRAPHIC ARTIST